Cannabis For Health Professionals:
Cannabis Harm Reduction
Did You Know?
Smoking remains the most prevalent and risky method of cannabis consumption.
Cannabis Resources:
Download the flash cards & graphs for in-office cannabis resources.
Cannabis Information for the Public
Cannabis Drug Interactions – Drugs.com
Cannabis Harm Reduction Resources for Healthcare Professionals
First legalized in 2018, New Brunswickers are now faced with a changing landscape of readily accessible cannabis consumption options. As cannabis consumption evolves, NB Lung recognized that there was a lack of accurate information and guidance surrounding cannabis usage and that harm reduction strategies could be used to limit its negative impact to New Brunswickers.
As smoking remains the most prevalent and risky method of cannabis consumption, the Cannabis Harm Reduction Program developed resources to give those working in health care settings a pathway to minimize potential harm. The goal of the program is to empower healthcare providers and patients alike to make informed decisions about cannabis use and its potential impact on health.
The Cannabis Harm Reduction Program by NB Lung was developed in collaboration with the New Brunswick Medical Society (NBMS).
About the Project
The Cannabis Harm Reduction Program is the result of a collaborative effort between NB Lung and the NBMS, building upon the success their “It’s your choice. Know the risks” public awareness campaign. Recognizing the significance of fostering open and informative conversations about cannabis, we have developed an array of resources to facilitate discussions between healthcare providers and patients.
Guiding Patients Down a Harm Reduced Path:
Understanding the time it takes for various methods of administration to take effect, and their duration, can be valuable when assisting patients in transitioning from smoking to less harmful ways of using cannabis. Many individuals opt for smoking cannabis because they prefer its rapid onset of effects, such as pain alleviation, psychoactive sensations, or the feeling of being “high.” In some cases, people might not even be aware of alternative consumption options.
If a patient’s daily routine and schedule allow for it—for instance, they have ample time and no imminent need to drive—a switch from smoking or vaping to using edibles or oils can mitigate the potential risks associated with lung health.
To illustrate, consider a patient who typically smokes cannabis before bedtime to aid sleep and won’t be operating a vehicle for the next 12 hours. Advising them to opt for a cannabis-infused edible instead of smoking provides a safer means of cannabis consumption that doesn’t compromise lung well-being.
Likewise, if a patient employs cannabis for pain relief and usually prefers smoking due to its swift onset, suggesting the use of a sublingual oil with a comparably rapid effect can offer a safer alternative.
Disclaimer:
Acknowledging limited available or conclusive research and significant information gaps in the field, our team has synthesized essential resources based on insights from a province-wide survey involving 1900 physicians and 235 nurse practitioners. Informed by an advisory committee encompassing physicians, medical students, nurse practitioners, and inputs from Indigenous communities, the resources are crafted to aid medical professionals in their efforts to safeguard lung health and reduce the potential risks linked to cannabis consumption. They are tailored to promote constructive discussions regarding cannabis usage and strategies for harm reduction so to guide patients toward adopting safer methods of consumption, facilitating the shift from smoking to alternatives like edibles and oils.
Due to limited research available, these resources are preliminary in nature and will be updated and revised as new peer-reviewed information becomes available. They serve as prompts, offering general guidance, to help primary healthcare professionals and patients start conversations about cannabis harm reduction.
Note:
Throughout the project, when we offer information about cannabis oil as an alternative to smoking, our primary focus is on sublingual oil and sublingual cannabis spray. We recommend sublingual oil because of its advantages, including quicker onset of effects, improved absorption, and precise dosing, especially when administered as a spray.
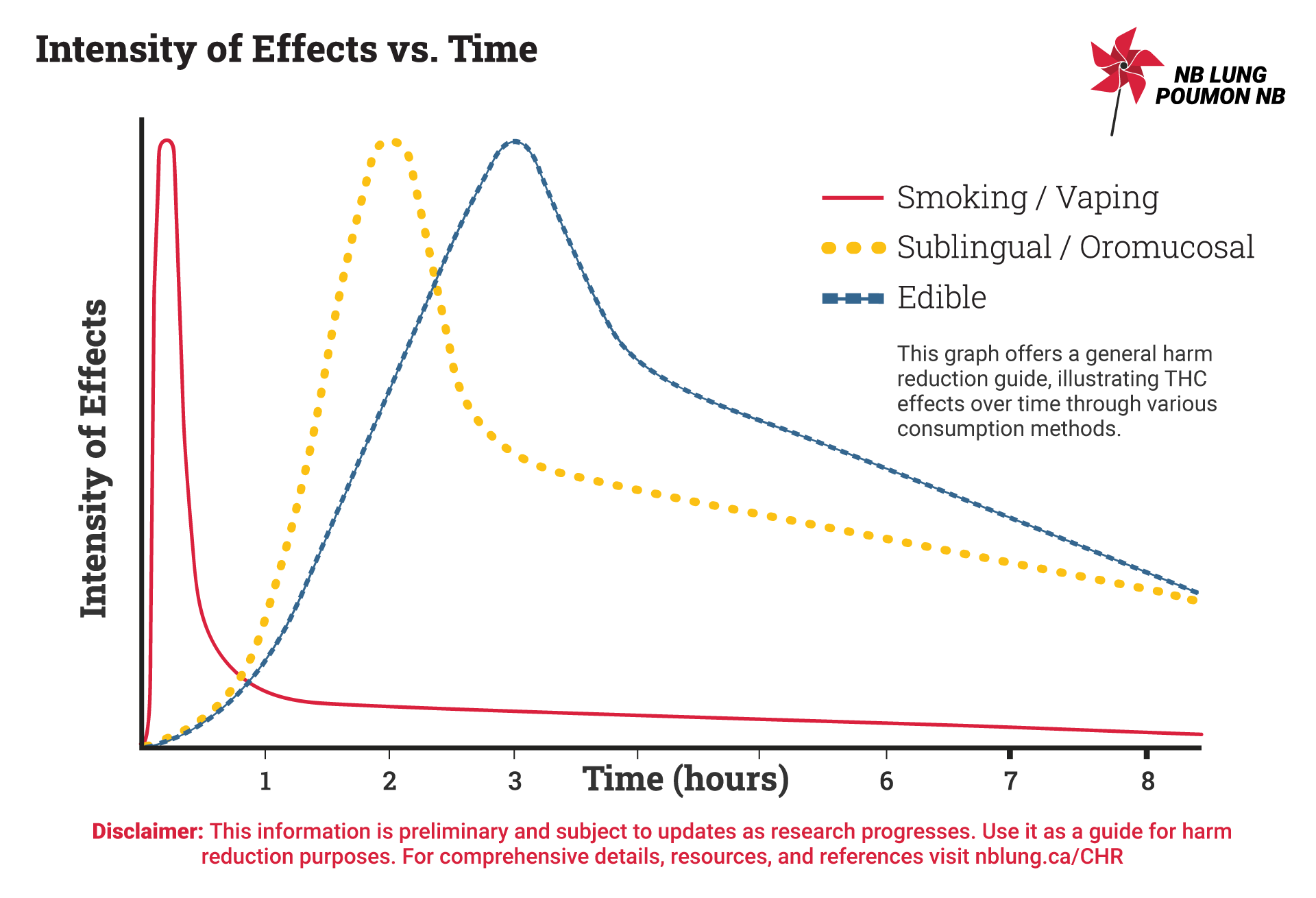
Intensity of Effects vs. Time
This graph visually depicts the effects of cannabis through various consumption methods, highlighting the times of onset, maximum intensity reached (based on peak plasma levels of THC) and duration of smoked cannabis, edible cannabis and sublingual cannabis oil.
The graph aims to provide a general understanding and it is important to note that these figures serve as guidelines rather than precise measurements due to variations in individual biology and differences in the routes of administration.
|
|
Time of Onset |
Max Reached |
Duration |
|
Smoking |
3-10min |
30min |
Up to 6hrs * |
|
Edibles |
30 min-2hrs |
2-4hrs |
Up to 12hrs * |
|
Oil (Sublingual) |
15-45min |
45min-4hrs |
Up to 12hrs * |
*Some effects could last as long as 24 hours
Graph and table adapted from 1, 2
About the Graph: Cannabis Pharmacokinetics
THC & CBD
- Cannabis contains a variety of cannabinoids, the most prominent being THC (tetrahydrocannabinol) and CBD (cannabidiol), which impact the body and mind in different ways. THC is psychoactive, while CBD is non-intoxicating. 1
- THC is the primary psychoactive component of cannabis and acts as a weak partial agonist on CB1 and CB2 receptors in the endocannabinoid system—a homeostatic regulator found in all chordates. THC influences pain, appetite, digestion, emotions, and cognition. ⁵12
- However, high THC content is associated with increased risks of adverse outcomes, both acute and chronic, including mental health issues and cannabis dependence. Psychoactive side effects vary depending on the dose and the individual’s tolerance history. For these reasons, THC is considered the optimal standard unit to measure cannabis exposure, particularly for safety assessments. ⁵,12
- CBD, on the other hand, has a non-psychoactive profile and provides potential therapeutic benefits across a range of conditions. It has shown efficacy in treating epilepsy, chronic pain, anxiety, and inflammatory and autoimmune conditions, and has properties including anticonvulsant, antipsychotic, neuroprotective, and anti-inflammatory effects. It can be used alone or in combination with THC. 12
- Medical cannabis patients, in contrast to recreational users, frequently use CBD-predominant chemovars with the smallest amount of THC to get the greatest improvement in symptom control, function, and quality of life, with fewest adverse events.¹²
- Notably, CBD may modulate the side-effect profile of THC, reducing the likelihood of adverse psychoactive events. Clinical recommendations—particularly for chronic pain—often base dosing protocols primarily on CBD levels, not THC. 35, 36
Inhaled Cannabis
- When cannabis is smoked, Delta-9-THC (Δ9-THC) quickly diffuses to the brain, eliciting a perceived high within seconds to minutes. Blood levels of Δ9-THC reach a maximum after about 30 minutes. Impairment is greatest during the first hour post dose and then rapidly subsides over the following 2-4 hours. ⁷,⁸
- The pharmacokinetics of vaporized and smoked cannabinoids are comparable. ⁹
Edible Cannabis
- The effects of eating cannabis are delayed, and the perceived high is relatively prolonged. The slow action of orally ingested cannabis is due to Δ9-THC being absorbed by the intestine and transported to the liver (hepatic first pass) where it is converted into 11-hydroxy-THC (11-OH-THC), an equipotent and longer-lasting metabolite. ⁷,⁸
- Following oral ingestion, psychotropic effects set in with a delay of 30 minutes to 2 hours, reach their maximum after 2–4 hours and last for about 12 hours, depending on dose and specific effect. ¹⁰,¹³
- The blood concentration of much more psychoactive 11-OH-Δ9-THC is much higher than after smoking .¹¹
- Following oral administration of CBD, a similar plasma concentration–time profile to that of oral THC has been observed ²⁰. Based on this profile, oral formulations may be useful for patients seeking symptomatic relief over a longer period.¹⁰
Sublingual Cannabis Oil
- Sublingual oil administration has a faster onset of action (approximately 15–45 minutes) and lasts similarly to the oral forms (6–8 h). ¹²
- Mean plasma levels reached the threshold of detection at 45 minutes after sublingual administration of a whole-plant cannabis extract containing THC. Higher concentration drops showed a later peak.¹⁴
Drug Interactions with Cannabinoids
As both THC and CBD are hepatically metabolized, the potential exists for pharmacokinetic drug interactions via inhibition or induction of enzymes or transporters.15 THC is oxidized by Cytochrome P450 enzymes (CYPs), including CYP2C9, CYP2C19, and CYP3A4. Therefore, serum levels may increase with inhibitors, or decrease with enzyme inducers.12 Pharmacodynamic interactions may also occur if cannabis is administered with other central nervous system depressant drugs, and cardiac toxicity may occur via additive hypertension and tachycardia with sympathomimetic agents.15
Pertinent drug interaction studies are few.16, 17 Existing studies have not demonstrated toxicity/ loss of effect of concomitant medications but are still theoretically possible.18 An important example is the CBD-mediated inhibition of clobazam metabolism.12,15 Cannabis is also purported to inhibit the metabolism of warfarin, increasing its anticoagulant effects.19
Further clinical studies in the actual patient populations for whom these drugs may be prescribed are needed to better understand their effects and ensure safe and effective use.15
Potential Pharmacokinetic Drug Interactions with THC & CBD
The following list includes, but is not limited to, potential pharmacokinetic drug interactions with cannabis and its effects on the bioavailability of THC and CBD. The drug interactions are highly variable on factors such as doses, administration routes, THC to CBD ratio and variability of cannabis products.
Certain medications of the following drug classes or molecules potentially increase the bioavailability of THC and CBD:
Bioavailability: refers to the extent to which a substance or drug becomes available to its intended biological target.
Potentially Serious Drug Interactions with CBD include:
Smoked marijuana can potentially increase clearance of these drugs:
Additional Drug Interaction Tables:
Cannabis: The Risks to Lung Health
Smoking and vaping cause harm to the lungs.
NB Lung’s goal is to provide physicians with the knowledge and tools to discuss these risks with patients and explore practical strategies for minimizing harm while promoting healthier choices.
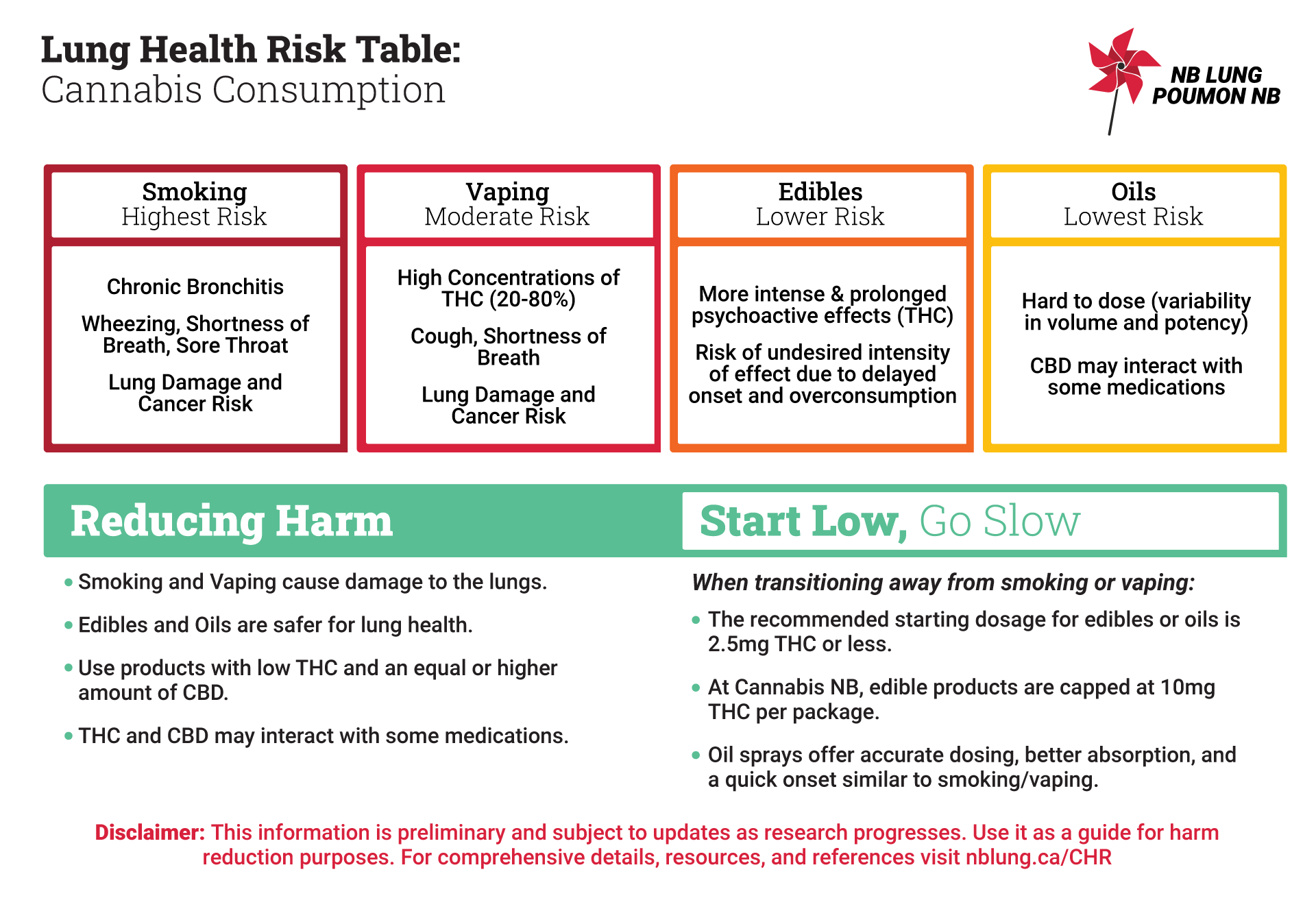
Lung Health Risk Table
| Smoking Highest Risk |
Vaping High Risk |
Edibles Lower Risk |
Oils Lowest Risk |
|
Chronic bronchitis²⁷ Cough, Wheezing, Lung damage and cancer risk²⁹ |
High Concentrations of THC (20-80%)³¹ Cough, shortness of breath¹² Lung damage and cancer risk²⁹ |
More intense and prolonged psychoactive effects (THC)⁶ Risk of undesired intensity of effect due to delayed onset and overconsumption³ |
Hard to dose (variability in volume and potency)¹² CBD may interact with some common medications ¹² ¹⁵ |
Detailed Consumption Method Facts and Risks:
Smoking
Prevalence and Potency:
• Smoking is the most common method of cannabis consumption. 39
• The average amount of cannabis smoked per day in Canada is 1.3 grams. 39
• Common joint sizes include 1g (1000mg), ½g (500mg), and ¼g (250mg). 39
• Joints sold at Cannabis NB typically contain 10–30% THC. 39
• Dried cannabis has a natural biological maximum of 30% THC (300 mg/g). 39
Risks:
• Smoke from cannabis combustion has been shown to contain many of the same toxins, irritants and carcinogens as tobacco smoke. 34
• Cannabis smokers tend to inhale more deeply and hold their breath longer than cigarette smokers, which leads to a greater exposure to tar per breath. 34
• Frequent cannabis-only smokers have more healthcare visits for respiratory conditions compared to nonsmokers. 30
Vaping:
Prevalence and Potency:
• Vaping cannabis results in 20–80% higher THC concentrations in the bloodstream compared to smoking.31
Risks:
• Vaping weakens the immune system and increases susceptibility to lung infection.34
• The perception of vaping as a safer alternative to smoking may encourage more frequent consumption or earlier initiation of cannabis, and a concomitant increased risk of developing problematic use or addiction.33 42
Edibles:
Prevalence and Potency:
• In New Brunswick, edible cannabis products are capped at 10 mg of THC per package.40
• A dose as low as 2.5 mg THC can produce psychoactive effects in some individuals.23
• It is recommended to start with no more than 2.5 mg and wait to feel effects before consuming more.3
Risks:
• Risk of accidental ingestion by children.3
Oils:
Prevalence and Potency:
• Oils and sprays allow for more precise dosing, especially oral sprays which deliver consistent doses. This makes it easier for users to control and monitor their intake.3
• Users are advised to consume no more than 2.5 mg of THC or one “activation” and wait before increasing dosage.3
• “Activation” refers to decarboxylation, the process that converts THCA to psychoactive THC. For instance, if an oil label says “8 mg THC per activation,” it delivers 8 mg of THC per spray or drop.3, 41
Risks:
• Both THC and CBD are metabolized in the liver, raising the potential for drug interactions due to enzyme or transporter inhibition or induction.15
Learn about drug interactions and cannabis.
Reducing Harm
Transitioning Away From Smoking
- Edibles and oils are safer for lung health²³
- Use products with low THC and an equal or higher amount of CBD¹²
- CBD can balance THC side effects, especially in daytime use, or when driving is required.¹²
- THC and CBD may interact with some medications¹² ¹⁵
- Medical cannabis patients, in contrast to recreational users, frequently use CBD-predominant chemovars with the smallest amount of THC to get the greatest improvement in symptom control, function, and quality of life, with fewest adverse events.¹²
Suggested Dosing for Harm Reduction:
Based on pharmacokinetic parameters like individual absorption, metabolism, sensitivity, tolerance, personal response to different consumption methods, etc., any dosages recommended are suggestions and guidelines and cannot be exact. Ultimately, starting with lower doses and gradually increasing as needed is recommended to find the appropriate dosage for desired effects while minimizing the risk of adverse reactions.²³
Start Low, Go Slow
The suggested approach to cannabis initiation is ‘start low, go slow, and stay low’.
- If smoking or vaping, suggest patient starts with 1 or 2 puffs of 10% (100mg/g) THC or less and wait 15 minutes. Then, they may increase by 1 inhalation every 15–30 min until desired symptom control has been achieved.¹² ³²
- If consuming edibles, suggest patient starts with 2.5 mg THC or less.¹² ³²
- Use products with low THC and an equal or higher amount of CBD¹²
- Sublingual oral sprays come in pre-measured doses, offering accurate dosing, better absorption, and a quick onset similar to smoking/vaping. ⁸ ¹²
- Learn about drug interactions and cannabis.
NB Lung has been helping New Brunswickers breathe easier since 1933.
Thank you for your support!
Page Last Updated: 28/02/2023